-
Property & Casualty
Property & Casualty Overview

Property & Casualty
We offer a full range of reinsurance products and the expertise of our talented reinsurance team.
Trending Topics
Publication
Recycling of Large Lithium-Ion Batteries From a Property Insurance Perspective
Publication
Looks Like Inflation Is Sticking Around. What Do We Do Now? [Part 3 of 3]
Publication
The Future of Cryptography and the Rise of Quantum Computing
Publication
Personal Injury Compensation in Europe: An Updated Comparison Among Different Systems Within the European Market
Publication
How to Plan for Cat Claims - Before, During, and After an Event -
Life & Health
Life & Health Overview

Life & Health
We offer a full range of reinsurance products and the expertise of our talented reinsurance team.
Training & Education
Publication
The Future Impacts on Mortality [Video]
Publication
Beware of Demo Mode on Electrocardiogram Reports
Publication
Understanding Breast Cancer in Asia – Awareness and the Importance of Screening
Publication
Marginal Gains in the Medicare Supplement Market U.S. Industry Events
U.S. Industry Events Moving The Dial On Mental Health
Moving The Dial On Mental Health -
Knowledge Center
Knowledge Center Overview

Knowledge Center
Our global experts share their insights on insurance industry topics.
Trending Topics -
About Us
About Us OverviewCorporate Information

Meet Gen Re
Gen Re delivers reinsurance solutions to the Life & Health and Property & Casualty insurance industries.
- Careers Careers
All in a Day’s Work – The Impact of Non-Medical Factors in Disability Claims

January 30, 2024
Mary Enslin
,
Lisa Hall
English
Inflation, worsening economic conditions, and increased cost of living were all daily headlines throughout the world in 2023. These adversities can make finding a job difficult when one is physically and mentally well; adding functional limitations can make it even more challenging.
According to the World Health Organization (WHO), diagnosis alone does not cause impairment or disability. Rather, disability results from the interaction between individuals, their health condition, and the personal and environmental factors within which they live.1 The WHO and many other organisations now recognise the importance of social determinants of health (SDOH). These are the myriad non-medical factors that influence health outcomes and include the environmental, social, and economic variables in which people are born, grow, work, live, and age, as well as the wider set of forces and systems shaping the conditions of daily life.
Research shows that these social determinants can be more important than healthcare or lifestyle choices in influencing health. For example, estimates show that the contribution of sectors outside health to population health outcomes exceeds the contribution from the health sector.2,3,4
Figure 1 shows the different categories of SDOH. It can be seen that healthcare quality and access is only one factor contributing to health, with economic stability, the environment, and the social context all playing equally important roles. We experienced this during the COVID‑19 pandemic, where many people reported being more impacted by lockdowns, inability to work, and worrying about the future than the direct physical effects of a coronavirus infection.6
Figure 1 – Social determinants of health categories

The role of work
If we accept that economic stability, the environment, and the social context are important social determinants of health, how do we incorporate this understanding into our management of Disability claims?
One significant activity that overlaps in all these areas, is work. Work is a central part of our lives. It is something we do almost every day, for much of the day, for decades on end. Recent estimates note that the average person will spend roughly 90,000 hours at work over their lifetime, one-third of their life!7
Compelling international evidence shows that in most circumstances, work is beneficial to people’s health and wellbeing.8 In addition to the salary earned, work gives us meaning and purpose, a way of structuring and occupying our time, physical and mental activity, opportunities to develop and use our skills, a sense of identity and personal achievement, social contact and support, and hopefully a feeling of accomplishment.
Conversely, people who are not in work have poorer physical and mental health overall, consult their doctors more frequently, are more likely to be admitted to hospital and have higher death rates. Some studies even go so far as to conclude that the risk to health of being out of work, in the long term, is greater than that of other major diseases such as heart disease. Therefore, many experts now recommend staying in work or returning to work as soon as reasonable following absence.
By taking a closer look at how work influences the social determinants of health, we can better understand the non-medical factors driving Disability claims and use this understanding to support claimants in returning to work.
Economic stability
The cost-of-living crisis seen in many regions around the world is impacting health and wellbeing, reinforcing the importance of economic stability. LifeSearch’s latest Health Wealth & Happiness Index, a UK survey commissioned with the Centre for Economics and Business Research, found that mental, financial, and physical health in 2023 deteriorated close to the “record low” levels recorded during the height of the COVID‑19 pandemic three years ago.
The index observed that almost one third (32 %) of British people experienced worsened mental health and wellbeing in the last year, with the cost of living crisis attributed as the biggest cause (44 %).9 In August 2023, the Inequalities in Health Alliance, convened by the Royal College of Physicians, published the results of polling commissioned from YouGov showing that of those who reported their health getting worse, 84 % said it was due to increased heating costs, over three quarters (78 %) said it was the result of the rising cost of food, and almost half (46 %) due to transport costs rising.10
Economic stability improves health, but barriers include lack of availability of work, childcare, career counselling, work flexibility, and availability of reasonable workplace accommodations.11 While insurers cannot directly impact broader economic conditions, we provide valuable services that contribute to economic stability. These include the financial protection itself, as well as services offered through claims management, such as vocational rehabilitation, wellbeing programmes, and recommendations around reasonable accommodations, to name a few.
Neighbourhood and built environment
While this category includes an individual’s residential neighbourhood and home conditions, given the amount of time spent at work, as well as the activities performed there, the physical work environment cannot be overlooked. Because people spend so much time working, their work environment has a major impact on their health. There have been situations where people develop hearing loss, skin diseases, or lung problems from exposure to risks at work, and musculoskeletal injuries remain a significant cause of claim in manual occupations.
While significant improvements in workplace health and safety have been implemented in the last 150 years, there is more that can be done. Interventions tailored to certain industries – such as efforts to prevent falls in the construction industry – can and have helped reduce work-related injuries, illnesses, and deaths. Almost every industry has seen significant changes due to new technologies, such as robotics and artificial intelligence. Employers can help improve people’s health and wellbeing by offering wellness programmes to promote wellbeing and prevent health concerns before they occur.12 Here insurers have valuable expertise to offer.
One significant recent change to work environments is the rise in remote working. In 2021, nearly three times more people were working in remote positions than in 2019.13 It is perhaps too early to judge, but some sources suggest this change may have a positive impact on health and wellbeing as individuals benefit from the flexibility and easier work-life balance. One survey in the UK found that workplace sickness absence recordings declined for the fourth year in 2023 alongside the growth in hybrid working.14
Social and community context
While physical injuries and illnesses may be decreasing, there is much discussion about the impact of work on our mental health. The social and community context is a term that refers to the settings and relationships in which people live and work, and how they affect their health and wellbeing. People’s relationships and interactions with co‑workers can have a major impact on their sense of cohesion and connectedness, which in turn impacts their health and wellbeing. The impact of workplace culture, communication, and discrimination, cannot be underestimated.15
Therefore, a thorough understanding of the insured’s workplace culture, wellness policies, and relationships is an important part of robust Disability claims management. In many cases, embitterment following conflict or perceived injustice in the workplace can present a bigger barrier to a successful return to work than the medical condition itself.
How to address the social determinants of health?
Claims professionals have little influence on the broader macro-environment, but we can have a significant impact on an individual’s ability to work, by preventing long-term absences and by supporting a return to work with comprehensive claims management after a absence.
If we accept that disability is impacted by the various social determinants of health, and we acknowledge that work is a significant source of these determinants, then it follows that robust and holistic claims management cannot focus on medical treatment alone. In many claims, it may be useful to incorporate non-medical strategies to complement traditional medical care and rehabilitation. Consider the following tools and resources:
Wellness starts before claim
The area of employee wellness has attracted more and more research over the past years. According to Deloitte, “as the line between work and life blurs, providing a robust suite of wellbeing programmes focused on physical, mental, financial, and spiritual health is becoming a corporate responsibility and a strategy to drive employee productivity, engagement, and retention.”16
According to Group Risk Development (GRiD), of the four key pillars of wellbeing – mental, financial, physical, and social – mental wellbeing is the number one priority that employees believe their employer should be responsible for supporting, with half (49 %) of employees choosing this over the other areas of wellbeing.17
Employers often turn to their insurers for advice and support regarding employee wellness. Where possible, insurers should look to support wellness programmes for both individuals and employers. This can take many forms, with common examples including wellness apps, employee assistance programmes, mental health counselling, and health monitoring and reward programmes.
The benefits of successful wellness programmes are multi-faceted. When wellness is prioritised, this results in a win-win-win outcome for the employee, employer, and insurer.
Understand the work related factors contributing to the claim
Best practice in Disability claims does not focus on medical information alone but includes an in‑depth understanding of the impact of the SDOH. While the ability to work is generally acknowledged to be a significant contributor to good health, risk factors at work are frequently cited as key precipitating and perpetuating factors for health problems.
Therefore, understanding and, where appropriate, addressing occupational factors is fundamental for robust claims management. Understanding the specifics of the insured’s occupation is paramount. The following factors are generally considered high risk:
- Jobs with inherently dangerous duties (e. g. oil rig workers, repetitive manual work)
- Jobs with high social and ethical responsibility (e. g. medical and welfare workers)
- Exposure to violence, trauma or abuse at work (e. g. healthcare professionals, police, military)
- Being self‑employed
- Employers with poor regard for employee wellness or negative workplace culture
- Work that is unpleasant or with low job satisfaction
- Work perceived as stressful – this is the most important
If a claim does occur, a thorough occupational and financial assessment is required. Work is far more than a job title, and a proper occupational assessment goes deeper than simply asking for a job title. It is crucial to understand the occupational demands of the job, as well as the physical and social environment of the workplace.
The level of detail required as part of the occupational assessment will depend on several factors, including the nature of the diagnosis and the expected duration of the claim, as well as the occupation itself. For example, if the insured has suffered a devastating accident and is currently incapacitated in hospital, it may be excessive and not fair treatment to the insured to insist on an in‑depth occupational analysis prior to deciding claim validity. On the other hand, if the insured is claiming for a more minor or subjective condition, a detailed analysis of the occupation may be vital. A good example is knee pain, which might not impair an accountant who can perform most of their duties while sitting but may be significant for a hairdresser who is required to stand for most of the day.
Consider reasonable workplace accommodations
The majority of absences are short-lived and most individuals return to work.18 A 2022 analysis of data from the UK’s Office of National Statistics noted that more than 26 % of people in the UK with long-term illness want to return to work.19 The article goes on to note that helping these individuals return to work will help the economy and assist employers with the staffing shortages they are currently experiencing.
Figure 2 – Accommodations for return-to-work or stay-at work
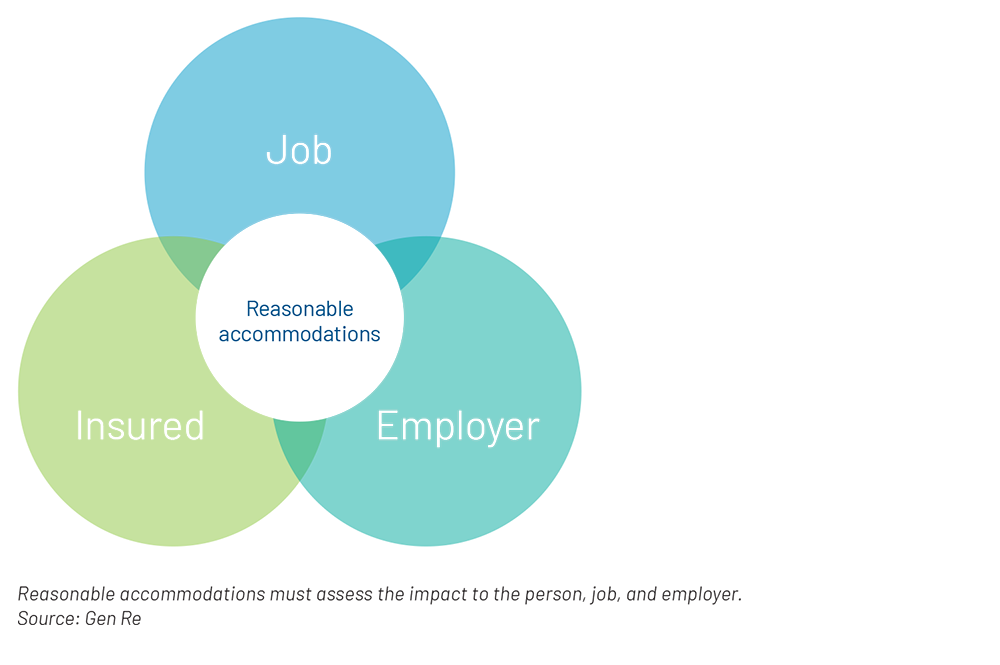
Additionally, vocational experts have found that by tapping into the expertise and knowledge of employees, employers save costs in onboarding and retraining because employees know the culture and the business, so everyone wins.
Returning to work or staying at work may involve providing reasonable accommodations. Simply put, this means that an employer will work with an employee to address the way work is performed – typically modifications or adjustments to the role, the work environment or the way things are done. These accommodations or modifications are often simple adjustments and may include aspects such as:
- Schedule changes
- Part-time or modified hours
- Job restructuring or carving out tasks
- Providing or modifying equipment
Accommodations are useful when:
- The insured has capacity but may not be able to perform their own occupation
- The attending physician(s) provides restrictions and/or limitations that are greater than the insured’s occupational requirements
- The insured does not have capacity but recovery is expected in the next three to six months
- The insured expresses an interest in returning to or staying at work
Occupational therapists and vocational rehabilitation counsellors are skilled at identifying occupational demands and potential ways to modify those requirements. They have access to tools and resources to assist in looking at tasks and job requirements and thinking about possible adjustments.
Let’s look at a few case studies where an accommodation assisted a person remain or return to work:
A truck driver has been diagnosed with PTSD and anxiety from his time in the military. He finds it challenging to go out in public and has to stop driving. His psychiatrist recommends he should consider a service dog to assist with his anxiety. The insured gets a dog and finds he is feeling better, but his employer has a policy that does not allow any animals in the truck. The insured and his vocational counsellor ask for a temporary trial allowing the service dog to ride along. The insured finds this works well and is able to return to work. The employer supports continued use of this accommodation.
An accountant has been experiencing low back pain and can no longer sit for more than 30 minutes at a time. She knows that she feels better when she has the ability to alternate sitting and standing. Her occupational therapist recommends a sit/stand workstation. This allows the insured to stay at work.
An attorney has carpal tunnel syndrome and was restricted from typing for more than 15 minutes out of every hour. Her occupational therapist suggested she should try a speech recognition application to assist with her typing. The insured learned how to use the software and found that even after she recovered from surgery, she was more efficient with the use of the voice recognition software and continued to use it. The new skill in this area helped her return to work earlier and improve her efficiency.
A warehouse worker has knee pain, he finds walking on cement floors increases his pain. His doctor suggested he consider anti-fatigue boots. Wearing these provides the relief he needs and the insured is able to continue in his role.
Consider coaching, mentoring or reskilling
Accommodations are not unique to individuals who are employees – those who are self-employed can also adapt how they do their work.It can be more challenging to think about different ways of performing work when self-employed because as humans we become used to doing things a particular way. In these instances, it might be helpful to consider utilising a coach, mentor, or consultant. Coaches and mentors may be professionally trained occupational therapists or vocational rehabilitation counsellors. Many Income Protection policies contain provisions that offer support for these types of services.
- Job coach: A job coach assists clients with assessing work skills in preparation for employment.
- Mentor: A mentor is a more experienced resource, providing expertise and knowledge to assist with skill development.
- Consultant: A consultant is typically a subject matter expert who assists clients in exploring employment options and goals, creating business plans, and identifying resources which help achieving those goals.
As more people become dependent on public government resources, concerns are rising around the world. In the UK a proposal has been made for general practitioners to refer their patients to life coaches rather than booking them off work. The idea is that life coaches can address the social determinants of health and assist patients with their general wellbeing, debt counselling, work conflicts, and other problems.20
Vocational counsellors are skilled at assisting with job-seeking skills, updating resumes, addressing interview questions, and conducting job searches. Things can change very rapidly in the world of work, so it may be beneficial to tap into a resource who can help navigate these waters, especially if a person has been out of work for a period of time.
In instances when an insured is unable to continue performing their occupation but continues to have capacity and wants to work, reskilling may be a good option. This may include looking at other roles within the same employer, or for a totally new employer or industry. In these situations, one typically begins by looking at the insured’s skills and work history for occupational alternatives. It could be they already possess the skills for alternative work, or they may need some skill development. If the skills the individual possesses do not translate to “gainful work”, exploration of retraining may make sense.
Conclusion
Understanding the social determinants of health is vital in the assessment of Disability claims. A good claims assessment considers not only the medical information submitted with the claim, but also the economic, social, and environmental impacts on a claimant. Once this understanding has been obtained there are many tools a claims professional can use to enable claimants to remain in work or return to work after illness or injury.
In some claims, simple workplace accommodations may be all that is needed. Others could involve more creative and complex work exploring coaching, mentoring, or reskilling claimants using occupational therapists, vocational counselling, life coaches or business consultants.
When claims professionals consider all factors that impact an individual’s health, we can provide a valuable, holistic, and personalised service to them that truly meets their needs.
Download PDF version for Endnotes.





